atient experience reflects the work we do. Here at Redstone Heath Center, we focus on everyone’s experience because we believe that ‘happy staff make happy patients.’ We take small, incremental steps every day, week, month, and quarter to improve our culture.
I (Teresa) started at Redstone 17 years ago as a medical assistant and continued working as an MA through nursing school. My late husband, who had type 1 diabetes, was very sick at the time. During his numerous health appointments, we noticed that the quality of care in the hospital and clinics fluctuated. This variability of care intrigued me, and I ultimately went into health care to give families a better experience than our own.
I’ve (Pati) worked in health care for 44 years, and I’ve been the manager at Redstone since 2000. A lot of what we do today are things we’ve done for years. The key to quality care is consistency. We don’t often say, “let’s try this tip or trick,” or, “let’s have a big kick-off.” Instead, we focus on small, sustainable actions that we can do consistently. I tell people that while it can be boring, but the small, sustainable things really do work.
1. Share patient feedback for learning, not shaming
We receive patient feedback from the patient experience team every week. These comments help us understand individual experiences and identify positive and problematic trends in patient care.
I (Pati) copy the patient comments into Epic and share them in a message with the entire clinic. We expect everyone—our front desk employees, medical assistants, and providers—to read patient feedback. While they may only check their email a few times a day, they live in Epic.
People now expect to see the comments. There will often be a conversation between the team —the medical assistants and the provider—to say “did you see that comment?” They investigate what a patient said to learn from the experience.
We encourage employees to view feedback as an opportunity for improvement. We don’t use patients’ comments to call out people for mistakes. We blame processes first, never people.
Our providers and medical assistants often use patient feedback as a platform to examine their concerns and learn from their experiences. If a comment refers to an MA or a patient relations specialist (PRS), one of us discusses it with them one-on-one. The conversation isn’t about whether or not it was the employee’s fault—it’s about helping them adjust their process.
When a patient expresses concerns regarding a provider, our previous medical director Dr. Mary Parsons (and now Dr. Sandra Van Leuven) stepped in to help. They approach the negative feedback as a coaching opportunity and holds peer-to-peer conversations with faculty members. Usually Dr. Parsons will come into our office to debrief on the patient and we look at their chart together to better understand the case
We look at negative comments like a case study and ask ourselves—what can we learn from this? If a patient comment includes a formal complaint or grievance that will go to the Customer Service department for response, we’ll discuss the comment in our management meetings. We talk about it, we investigate the chart. We don’t want to overly react, but instead treat it like a case study.
2. Reserve time to talk through trends
We hold brief quarterly one-on-ones with every member of the team. Technically, its only three— number four is the MA and PRS annual evaluation. Each quarter, we start with the providers and the medical director leads those meetings. They are only about 30 minutes, and we go over patient experience, quality, and finance. We catch up what is going on with their practice, and if they feel like there is anything that needs to be addressed with the rest of the team. We start with the providers so if there is something we want to bring up with an MA, we know that in advance of their one-on-one.
The rest of the staff one-on-ones are usually 15 minutes or less. If we’ve seen a pattern of behavior, we address when we see it, not wait for a quarterly one-on-one. We never mix disciplinary action with one-on-ones. We want everyone to feel safe coming to our office. At our quarterly one-on-ones, we talk about how they’re doing.
We review the individual’s patient experience, quality, and finance, compared to the rest of the clinic. Our one-on-ones are strictly to go over what is on the agenda. Usually, we’ve identified a trend earlier, like missed punches, so when it comes to the employee’s quarterly one-on-one, we can comment on the improvement and highlight the positive actions. We hold the meetings during the first few weeks of the quarter. If we’re late scheduling them, staff usually ask us—“when is my one-on-one?” It’s a positive meeting.
3. Create a culture of thank you
Consistent actions create an environment of engagement, and most of those actions focus on increasing positivity and recognizing people. When an employee joins, we have a brief introduction to patient experience. We let them know what it is and how we measure. In addition to sharing patient comments every week, we also post updated scores from the system patient experience team. When we look at these comments, we don’t just ask, “How can we improve?” We also want to recognize what we are doing well, both as individuals and as a whole.
We actively thank people every week. If a comment specifically praises one of our staff members, we send that employee a handwritten card from our management team. Even if the patient’s message is as simple as: "We love Cheryl," we write her a little note saying, "We love you too. Thank you for taking such great care of our patients." We mail those notes to their house.
We also realize the importance of peer-to-peer appreciation. As management, we don’t always see the everyday things that the team does for each other. For the last six years, we’ve held a “Thankful Thursday” huddle where employees can share why they are thankful for their coworkers. We read their messages aloud and give small treats, like candy, to the person who is being recognized.
We post those thank-you messages to a bulletin board. During different seasons, we arrange the messages in fun shapes like mittens or footballs. When we change up the board, it revitalizes everyone and motivates them to help contribute to the new design.
People often tell us that the culture feels different at Redstone. We believe it all comes back to our staff. When a new employee joins the team, everyone wants to take them under their wing and help them succeed. We’ve created a culture of caring for one another; we recognize and reward each other for helping. We take care of ourselves, so that we can take care of each other, so that we can take care of our patients.
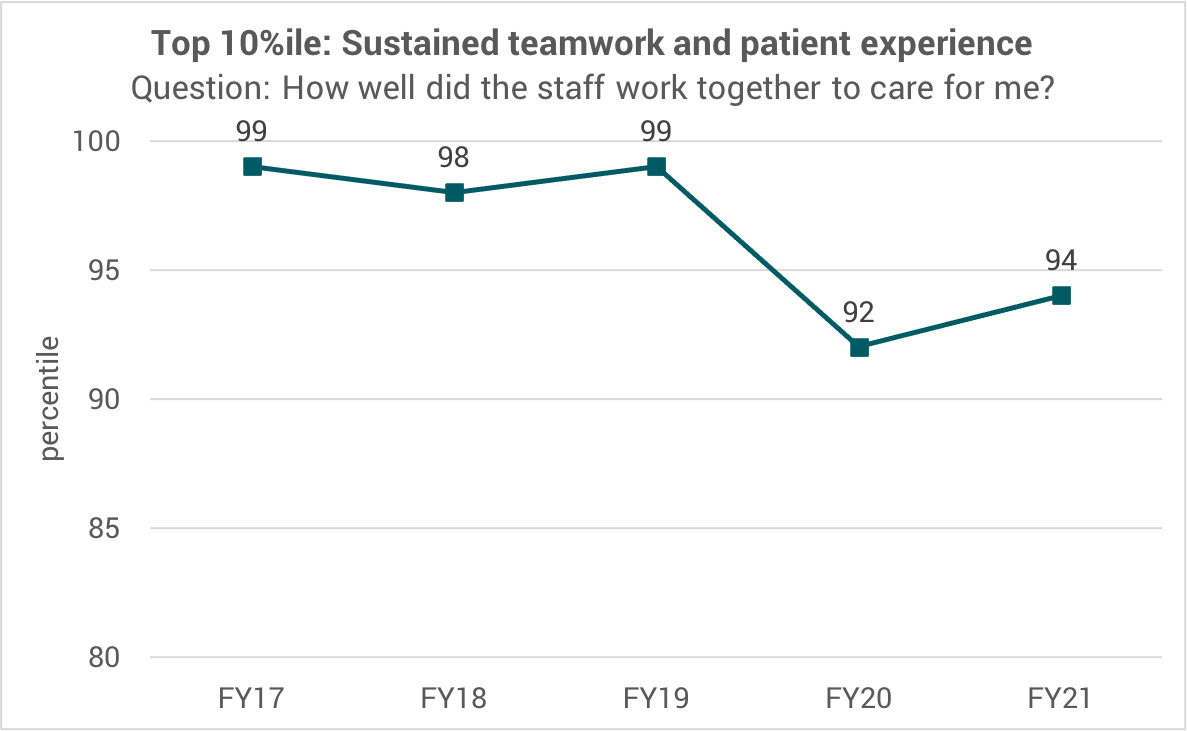
Source: U of U Health Patient Experience office. Press Ganey survey data by received date; Percentile; UHC Benchmark.
Pati Colvin
Teresa Stone
Urogynecology specialist Whitney Hendrickson-Cahill details the steps an interdisciplinary team followed to reduce surgical site infections (SSIs) following hysterectomy procedures, aiming to improve patient outcomes, shorten recovery times, and reduce healthcare costs at University of Utah Health.
Former Chief Quality Officer Sandi Gulbransen and Accreditation Manager Kemper Funk explain how this umbrella of standards—ISO-9001—relates to our accreditation process and impacts our daily work.
Pediatric hospitalists and patient advocates Reena Tam and Erin Avondet shed light on the untapped opportunity to augment pediatric vaccination coverage in our communities and build vaccine confidence in the inpatient setting. They provide a host of resources and practical tips you can apply right now.
